How to Deal with a Crick in the Neck: Effective Remedies and Prevention Strategies
A crick in the neck is a common and often bothersome condition that many of us have experienced at one point or another. It usually manifests as a sharp pain…
Deep Knots in Shoulder Blades: Symptoms, Causes, and Treatment
Shoulder discomfort is a common issue that can arise from various causes, and one prevalent complaint is the presence of deep knots in the shoulder blades.…
Turtle Neck Syndrome: Causes, Symptoms, and Solutions
What is Turtle Neck Syndrome?In today’s digital age, it’s common to find ourselves glued to our screens for prolonged periods, whether it’s for…
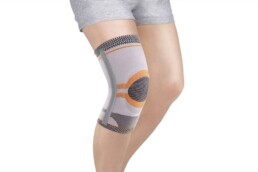
Best Knee Wrap for Baker's Cyst: a Guide
What is a Baker’s cyst?A Baker’s cyst is a fluid-filled sac that develops on the back of the knee due to an excess of the synovial fluid that lubricates the…
Pulled Glute Muscle: How to Treat a Pulled Gluteus Maximus
Your gluteus maximus is a powerful muscle that helps you perform many everyday activities. It’s easy to take this muscle for granted until it starts to…
Hypertonic Pelvic Floor
A hypertonic pelvic floor refers to the condition where the muscles in the pelvic floor are constantly tightened or contracted. This continuous contraction may…
Difference Between Swedish and Deep Tissue Massage
Swedish and Deep Tissue are two popular types of massage therapies. While they may seem similar at first glance, there are key differences between the two. A…
Car Accident Physical Therapy: a Patient Guide
Car accident physical therapy, also known as auto accident rehabilitation, is a specialized form of therapeutic intervention. It’s designed to reduce…
Things to Avoid with Degenerative Disc Disease
What types of physical activities should I avoid with Degenerative Disc Disease?It’s crucial to note that while regular moderate exercise is beneficial…
Ball of Foot Pain: a Guide to Causes
Why Does the Ball of My Foot Hurt?The ball of your foot, the pad just behind your toes, is vulnerable to different injuries and conditions which can result in…
Neck Pain from Sleeping
Neck hurts after sleeping: what are the most common causes?Neck pain after sleeping is not an uncommon experience for many individuals. It is often caused by a…
Why Is It Hard To Stand Up After Squatting?
Why Squat Anyway?As you get older or are more sedentary after working from home throughout the pandemic, it may seem more difficult to stand up straight after…
What is Tendinitis?
If you’ve heard people talk about suffering from tennis elbow or runner’s knee, they’re referring to forms of tendinitis. Tendinitis is an inflammation or…
Understanding Active Release Technique
If you’re suffering from a sports injury, an overuse impairment or chronic pain, it can be helpful to consider therapy in the form of Active Release Technique…
What to Do for a Stiff Knee
It’s no fun to have a stiff knee or to feel aches and pains in your knee joints. Knees are so central to our ability to move easily, that any hiccup in their…
Working from Home Ergonomics: A Guide to Preventing Injuries
As the days of the pandemic turned into months, it became obvious to Canadians working from home that their makeshift office settings were leading to…
The Benefits of Physical Therapy Throughout Your Life
Many people associate physical therapy with injury. You see your physical therapist when you’ve sprained an ankle playing tennis or injured a knee while…
New Mother Aches and Pains: How Physiotherapy Can Help
Pregnancy is a wonderful, joyful time for many expectant mothers, but it can be accompanied by a slew of physical discomforts: heartburn, headaches, morning…
The Scoop on Overuse Injuries
As research has shown, exercise is extremely beneficial for both our body and our mind. It keeps the body strong and healthy so it can fight off illness…
Preventing Back Pain for Flight Crews and Travellers
Air travel is a fact of life for many of us, whether because it’s our livelihood, our work demands it or we want to explore places that are most easily…
Warehouse Work Causing Back Pain
With the rise of Internet shopping, the warehouse – and the warehouse worker – has become a more visible part of the supply chain. When…
Why are my shoulders sore?
You’ve heard your friends describe someone by saying, “He carries the world on his shoulders.” It’s a saying that derives from Greek mythology and it refers to…
What Causes Neck Pain?
At one time or another, you’ve undoubtedly muttered to yourself, “What a pain in the neck.” Of course, you’re generally referring to an annoyance, not to a…
How to Manage a Shoulder Separation
References to shoulders generally touch upon strength: shouldering a burden requires it, as does carrying the weight of the world on your shoulders. However,…
How to Avoid Accidents This Winter
As fall shades into winter, we slowly adjust to the changes in the weather: the colder temperatures, the darkness that greets us each morning and falls early…
Stay Fit During the Winter
As the days get shorter and the outdoor temperature drops, there’s no avoiding the truth: Winter is coming. Many of us dislike the combination of dark and cold…
Piriformis Syndrome - a real Pain in the Butt
We’ve all heard people say it, no matter how impolite it may sound, “What a pain in the butt!” However, anyone who is suffering from piriformis syndrome can…
Tailbone Pain: How can I relieve it?
The technical term for the tailbone is coccyx, which is derived from the Greek word for cuckoo. It was so named because the bone resembles the shape of the…